
Ultimate Guide to Nursing Specialties
Emergency Room (ER)
Are you interested in ER nursing? Read on for the ultimate guide to this nursing specialty: certifications, salary, challenges, and more.
Intensive Care Unit (ICU)
What does ICU mean in medical terms? Short for intensive care unit—learn more about the ICU nursing specialty in this guide.
Acute Care
Are you looking for flexible, high-paying acute care nursing jobs? Read on for an overview of working in hospitals as a per diem nurse, CNA, or PCT.
Skilled Nursing
What is skilled nursing? Learn more about skilled nursing care and facilities and find key considerations for nurses and healthcare professionals.
Medical Surgical
Want to know more about med-surg nursing? This comprehensive guide covers the skills, salary, and responsibilities of medical-surgical nurses and CNAs.
Gynecology
Explore the full scope of gynecology, from preventive screenings and managing PCOS to advanced minimally invasive surgery and key subspecialties.
Respiratory Therapy
Explore the vital role of respiratory therapy. This guide covers the RT's scope, key interventions, and critical impact on patient outcomes in healthcare.
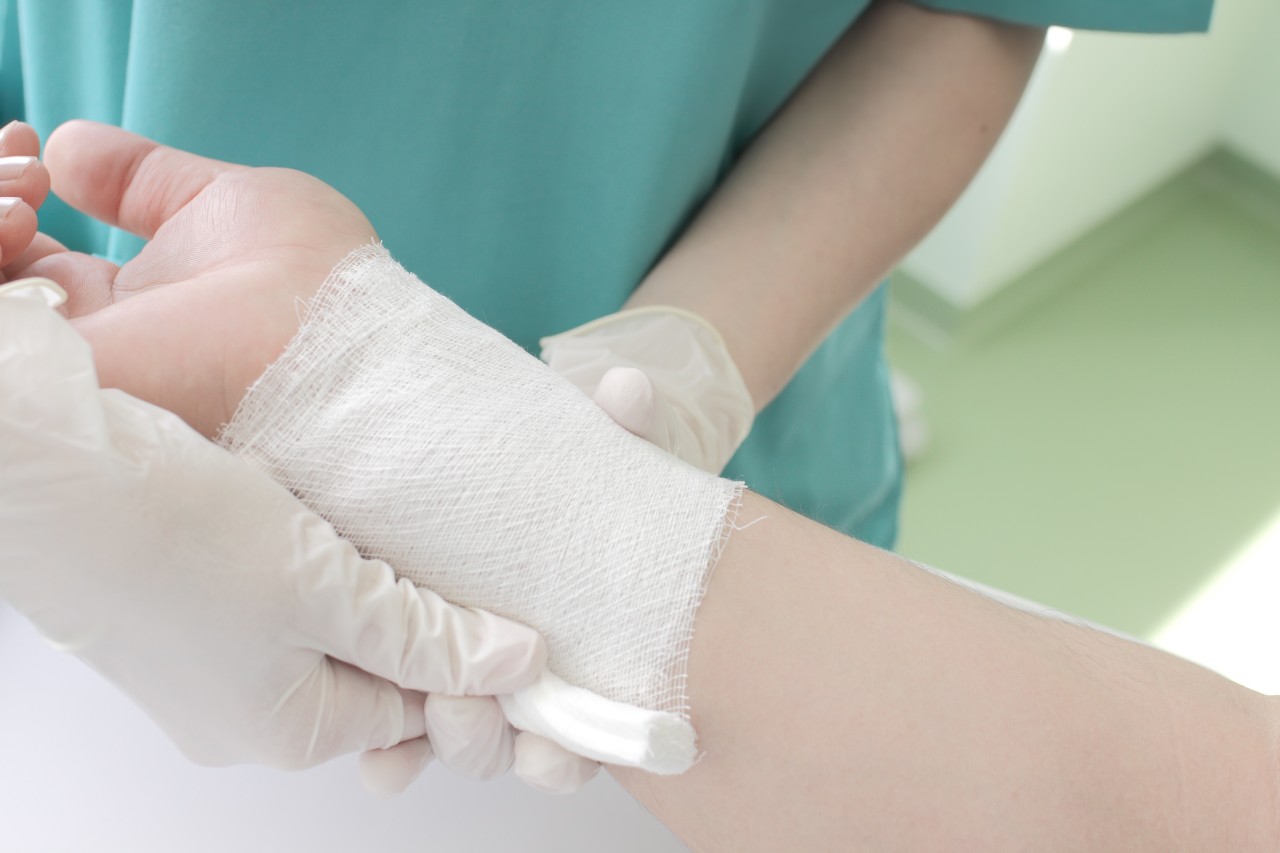
Wound Ostomy Care
Explore wound, ostomy, and continence care. Our guide covers key services, clinical practices, and how this specialty improves patient outcomes and facility performance.
Hematology/Oncology
Explore hematology/oncology services, disease types, diagnostics, treatments, and care team roles across modern cancer and blood disorder care.
Hematology
Hematology is essential. Understand blood disorders, advanced diagnostics, and treatment options impacting care teams across your facility.
Allergy and Immunology
Explore the allergy and immunology service line. This guide covers diagnostics, treatment protocols, and operational strategies.
Urology
Explore a comprehensive overview of urology services, from clinical practice and patient care to operational management and new innovations.
Otolaryngology (ENT)
Go beyond surgery. Otolaryngology restores essential functions like hearing, breathing, and voice with team-based care for chronic ENT conditions.
Orthopedics
Learn how rheumatology addresses autoimmune and joint disease, chronic pain, and infusion treatments—what this specialty means across today’s healthcare landscape.
Dermatology
Explore dermatology roles, workflows, technology, safety, and practice management strategies that support high-quality patient care across clinical settings.
Rheumatology
Learn how rheumatology addresses autoimmune and joint disease, chronic pain, and infusion treatments—what this specialty means across today’s healthcare landscape.
Neurology
Understand how neurology evaluates and treats disorders of the brain, spinal cord, and nervous system through advanced diagnostics, clinical care, and research.
Infectious Diseases
Essential guide to the infectious diseases specialty: core management strategies, multidisciplinary teams, quality improvement, and facility administration.
Gastroenterology
Explore gastroenterology’s impact on care, operations, and teamwork—from acute GI emergencies to chronic management—serving clinicians and facility leaders.
Endocrinology
Optimize your endocrinology practice with best practices for workflow, staffing, precise billing/coding, and technology.
Gerontology/Geriatric Medicine
Discover the future of elder care. This guide covers geriatric care management, patient safety, and technology integration for aging populations.
Pulmonology
Pulmonology: Critical teams, advanced diagnostics for respiratory care, chronic disease, and pandemic response.
Cardiology
Explore the evolution of cardiology throughout history. Discover how modern approaches and technology enhance heart care for improved patient outcomes.
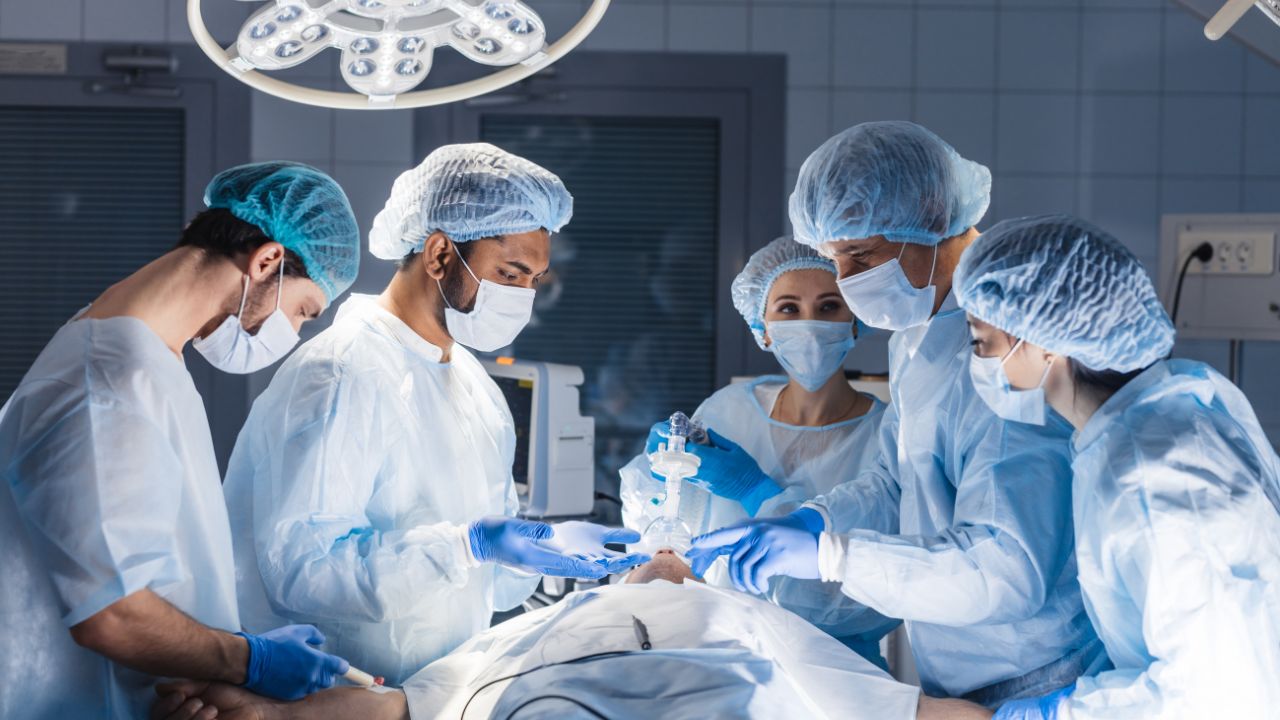
Anesthesiology
Anesthesiology is more than the OR. Discover its role in safety, tech, pain management, and ICU leadership. A look at the modern perioperative strategist.
Critical Care/Intensive Care
Explore critical care roles, ICU staffing, protocols, leadership, and evidence-based systems that support safe, reliable intensive care in high-acuity settings.
Nephrology
Explore nephrology’s vital role in healthcare, bridging acute care with chronic management. Essential insights for clinicians and facility leaders.
Primary Care
Primary care is the cornerstone of healthcare, offering comprehensive services from prevention to chronic disease management.
Emergency Medicine
Master the critical seconds: Explore 24/7 rapid decision-making, multi-disciplinary collaboration, and the life-saving protocols of acute emergency care.
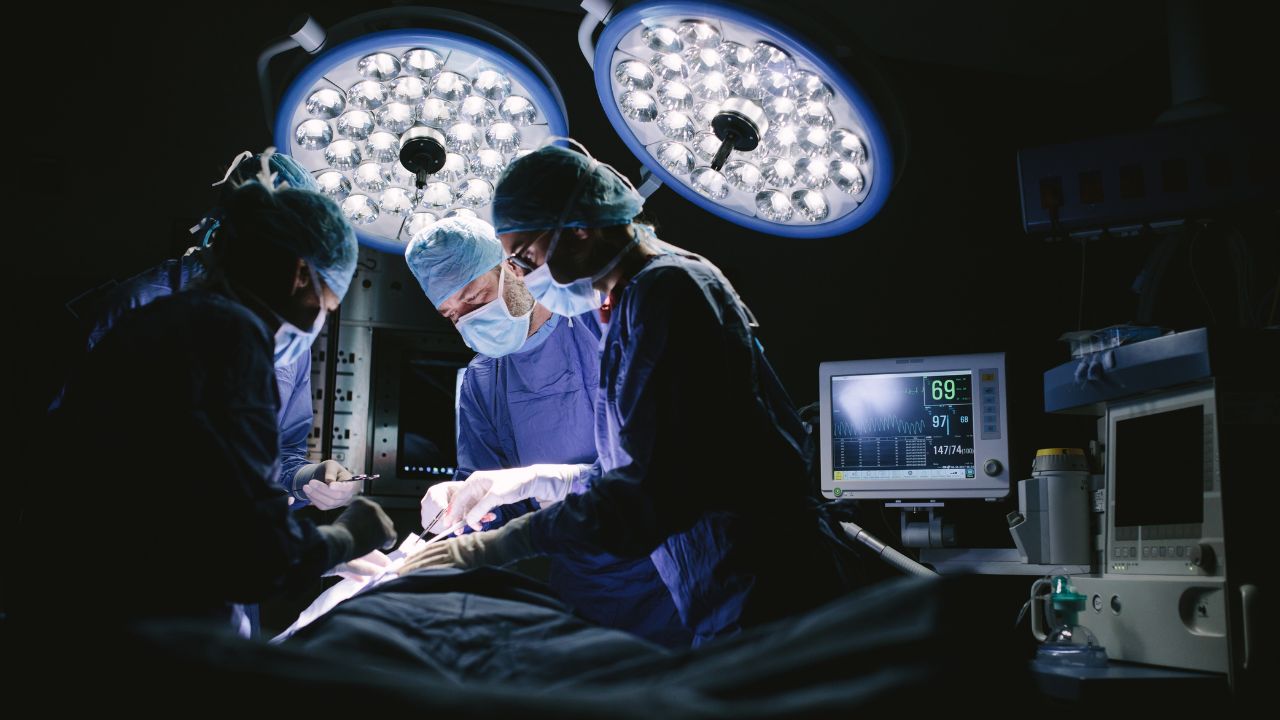
Surgery
Are you thinking about giving operating room nursing a try? First, read on to learn all there is to know about this nursing specialty.
Psychiatric Unit
Are you interested in psych nursing? Find the answers to all your questions in this ultimate guide to psychiatric nursing.
Long Term Acute Care Hospital
What is a long-term acute care hospital? How does it differ from other hospitals and long-term care facilities? Learn about LTACHs here.
Inpatient Rehab
Are you a healthcare professional trying to understand your career options? Inpatient rehab may mean more than you think. Discover all the uses of this term.
Telehealth
Have you ever considered a career in telehealth nursing? Read on to learn about this career path. It just might be perfect for you!
Progressive Care Unit
Are you a newly graduated nurse exploring career options? Read on to learn all there is to know about the progressive care specialty.
Wound Care
Are you interested in wound care nursing? This ultimate guide to wound care nursing covers everything you need to know about this specialty!
Endoscopy
Would you like to learn more about endoscopy nursing? In this ultimate guide, you will find everything you need to know about this specialty
Disaster Response
Are you interested in disaster response nursing? Read on to learn all there is to know about this indispensable nursing specialty.
Psychiatric Unit Nurse
Are you interested in psych nursing? Find the answers to all your questions in this ultimate guide to psychiatric nursing.
Dialysis
Are you interested in dialysis nursing? Read on for the most comprehensive guide to nephrology nursing on the web today!
Peds Telemetry
Want to learn more about the ped tele nursing specialty? Find find nearby peds tele PRN nursing jobs and why nurses love this specialty.
PICU
Want to learn about the pediatric ICU (PICU) nursing specialty? Find everything you want to know about this area in our ultimate guide.
Mother/Baby
Are you considering a career in mother and baby nursing? Read on to learn everything about postpartum nursing in this comprehensive guide.
Case Manager
Are you considering working as a case manager? Read on to learn everything there is to know about case management in this ultimate guide.
Home Health
Are you wondering if home health nursing is right for you? Find the most comprehensive guide to this nursing specialty on the web today.
Long Term Care
Are you interested in a career in long-term care (LTC)? You have come to the right place. Read on for the most comprehensive guide for this nursing specialty.
Respiratory Nursing
Are you interested in respiratory nursing? This ultimate guide covers everything there is to know about this essential nursing specialty.
Pediatric
Want to learn about the pediatric nursing specialty? RNs, LPNs, & CNAs who like working around children enjoy picking up PRN Peds jobs.
Behavioral Health
Are you considering a career in behavioral health nursing? Learn everything there is to know about this essential nursing specialty.
Neonatal Nursing
Are you curious about neonatal nursing? This ultimate guide to working as a neonatal nurse covers all there is to know about this specialty.
Nurse Practitioners
What is a PRN or travel nurse practitioner? Learn more about this medical specialty and why people choose this healthcare career.
Rehabilitation
What is the rehabilitation nursing specialty? Learn more about working in rehab and what nurses and clinicians are in this field.
Hospice
Are you considering hospice nursing? Learn the pros and cons of hospice nursing and everything else you want to know about hospice care.
Pediatric ER
Want to learn more about the pediatric emergency room specialty? Find out what types of nurses work here & find local PRN peds ER jobs.
Assisted Living
Assisted living facility something you are considering? Learn everything you need to know about this nursing specialty.
Labor & Delivery
This labor and delivery nurse guide can help you understand what this specialty is like, how much L&D nurses make, and where to find high-paying jobs.
Radiology
Discover how radiology impacts modern medicine and learn about radiologist roles, safety protocols, and innovations in radiology.
Cardiovascular Nursing
Are you interested in working in the cardiovascular intensive care unit as a registered nurse? Learn how to become a CVICU nurse and what this role entails.
OR
Are you thinking about giving operating room nursing a try? First, read on to learn all there is to know about this nursing specialty.
Oncology
Are you interested in oncology nursing? Read on to learn everything there is to know about this essential nursing specialty.
PACU
Want to learn about the post anesthesia care unit (PACU) nursing specialty? Learn more and discover PACU RNs, LPNs, & CNAs jobs near you.
Pediatric Surgery
Want to learn more about the PED OR nursing specialty? Find out what drives nurses to work in this field and view RN PRN jobs in peds OR.
Pre-Operation
Are you wondering what pre-op nursing is? Learn about this specialty's job duties, pros and cons, salary information, and more in this resource guide.
Ventilator Care
Nurses in this specialty must be highly skilled and knowledgeable in the use of pulmonary equipment and monitoring techniques.
Continuing Care Retirement Community
A continuing care retirement community is a type of retirement home that offers a combination of housing, services, and healthcare treatments.
Urgent Care Nursing
Have you ever considered working as an urgent care nurse? This ultimate guide covers everything you need to know about urgent care nursing.
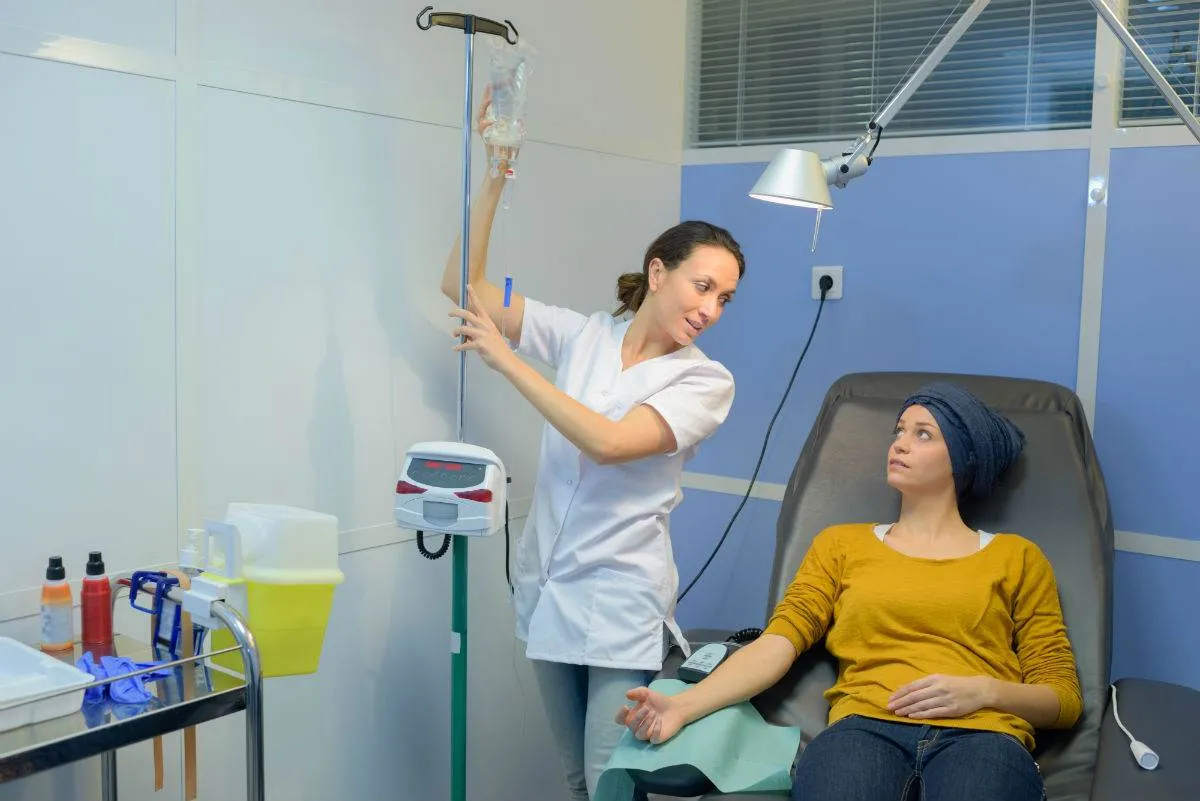
Chemo Infusion
Are you interested in chemo-infusion nursing jobs? Discover how to become a chemo-infusion nurse, average salary, typical duties, and more.
Telemetry
Do you have questions about telemetry nursing? Look no further. Here are answers to both simple and technical questions regarding this in-demand specialty.
Obstetrics Nursing
Are you considering a career in OB/GYN nursing? Read on to learn all about this essential and highly desired nursing specialty.
Dermatology
Dermatology nursing covers everything from cosmetic procedures to treating life-threatening conditions. Learn more about dermatology nursing here.
Nurse-Midwife
Are you a nurse and passionate about childbirth? Learn about the certified nurse midwife (CNM) specialty to help you decide if it is the right career path for you.
Intermediate Care
Intermediate care nursing is a specialty that focuses on providing skilled nursing care to medically stable patients with complex medical conditions. It connects home and acute care.
Geriatric
Geriatric nursing is a specialty that focuses on delivering care to persons of older ages. Learn the definition, meaning, and skills to work in geriatrics.
Occupational Health Nursing
Ever considered occupational health nursing? This specialty may not be the most traditional nursing role, but it just might be perfect for you!
Catheter Laboratory RN
Are you interested in cardiac cath lab nursing? Find the answers to all your questions about cath lab and more in this ultimate guide.
Flu Crew Nurse
Wondering what it’s like to work as a flu vaccination nurse? Read on for the most comprehensive guide on flu shot nursing on the web today!
Step Down Unit
Step down unit nursing is a specialty that focuses on providing nursing care to patients who are in the transitional stage between acute care and a lower level of care.
Flight Nursing
Are you a nurse who loves to fly? Flight nursing may be the perfect career choice for you! Read on to learn all there is to know about this nursing specialty.
Memory Care
Are you a newly graduated nurse exploring your career options? Learn all about memory care and the role of nurses in this specialty.
Med/Surg TELE
Med-Surg Tele Nursing Specialty offers nurses the opportunity to provide high-level care to patients on med-surg units who require a nurse specialized.
Physical Therapy
Physical therapy restores function, enhances recovery, and supports success in clinics and facilities—empowering clinicians, managers, and improving patient care.
Electronic Intensive Care Unit
An electronic intensive care unit (eICU) is a specialized type of telemedicine system in which remote critical care physicians monitor patients in various settings.
Read more about it




.jpg)







.webp)
















































Popular Topics
Start exploring PRN jobs opportunities here
These quick links are here to streamline your search and discover a range of opportunities tailored to your preferences.

Pick Up a Job Today
Find per diem PRN job opportunities in your area. High paying CNA, LPN and RN and many more licences are available now.
Join NursaPost Your Jobs Today
Facilities who use Nursa fill 3 times as many open per diem shifts, on average, compared to trying to fill the shifts themselves.
Post JobsSelect your license and location to find the best PRN jobs
Select your license and the location you want to work in, and we'll show you the best PRN jobs available nearby.













.webp)







